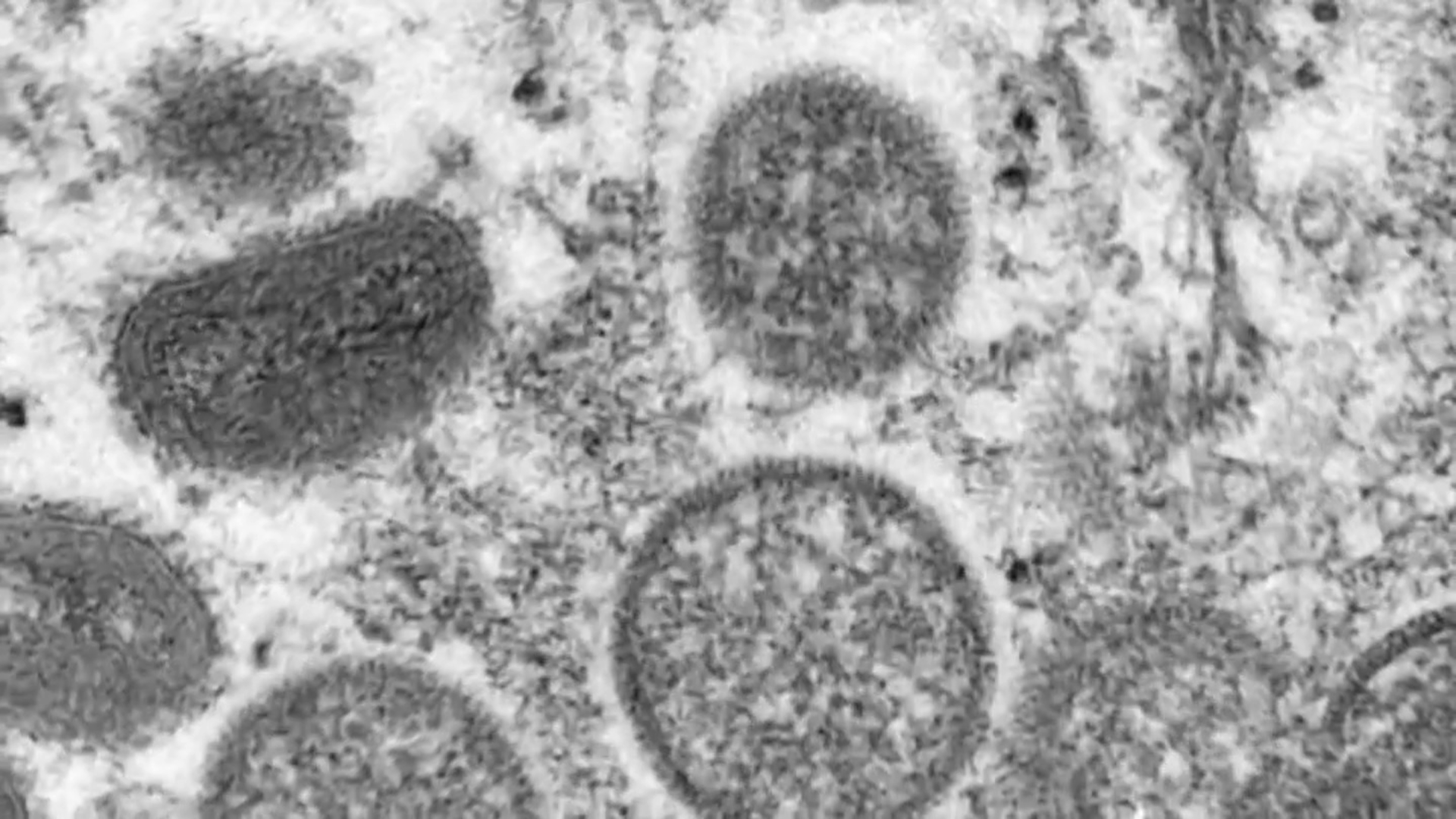
U.S. health officials on Tuesday authorized a plan to stretch the nation’s limited supply of monkeypox vaccine by giving people just one-fifth the usual dose, citing research suggesting that the reduced amount is about as effective.
The so-called dose-sparing approach also calls for administering the Jynneos vaccine with an injection just under the skin rather than into deeper tissue — a practice that may rev up the immune system better. Recipients would still get two shots spaced four weeks apart.
The highly unusual step is a stark acknowledgment that the U.S. currently lacks the supplies needed to vaccinate everyone seeking protection from the rapidly spreading virus.
That includes 1.6 million to 1.7 million Americans considered by federal officials to be at highest risk from the disease, primarily men with HIV or men who have a higher risk of contracting it. Vaccinating that group would require about three times more full doses than the roughly 1.1 million that officials have made available.
Get New England news, weather forecasts and entertainment stories to your inbox. Sign up for NECN newsletters.
The White House’s monkeypox response coordinator, Robert Fenton, said the plan would help the U.S. “stay ahead of the virus.”
“It’s safe, it’s effective, and it will significantly scale the volume of vaccine doses available for communities across the country,” Fenton told reporters.
The Biden administration declared monkeypox a public health emergency last week in an effort to slow the growing outbreak that has infected more than 8,900 Americans. Officials announced a separate determination Tuesday that allows the Food and Drug Administration to expedite its review of medical products or new uses for them, such as the dose-sparing technique for Jynneos.
The FDA authorized the new approach for adults 18 and older who are at high risk of monkeypox infection. Younger people can also get the vaccine if they are deemed high risk, though they should receive the traditional injection, the agency said.
The announcement represents an about-face from last month, when the FDA and other agencies repeatedly stressed that two full vaccine doses were necessary for adequate protection.
But regulators now point to a 2015 study showing that vaccination with one fifth of the traditional dose generated a robust immune-system response comparable to that of the full dose. About 94% of people receiving the smaller dose had adequate levels of virus-fighting antibodies, compared with 98% of those receiving the full dose, according to the study funded by the National Institutes of Health.
The NIH is planning an additional trial of the technique in coming months, according to the agency.
Vaccine makers often formulate their shots to provide more than enough protection, so it's not unusual that a smaller dose could still prove effective.
But some experts and advocates warned there is little data to support the policy and worried it could backfire if it reduces the vaccine's effectiveness.
“We have grave concerns about the limited amount of research that has been done on this dose and administration method, and we fear it will give people a false sense of confidence that they are protected,” said David Harvey of the National Coalition of STD Directors, in a statement.
The smaller doses also require a different type of injection that penetrates only the top layer of skin, rather than the lower layer between the skin and muscle. That's a less common technique that may require training for some health practitioners. It's also associated with more side effects such as redness, itchiness and swelling.
The shallower injection is thought to help stimulate the immune system because the skin contains numerous immunity cells that target outside invaders.
The Centers for Disease Control and Prevention said it will provide educational materials on the technique along with a broader awareness campaign for U.S. health departments.
Rationing vaccine doses is common in Africa and other parts of the world with limited health resources. In recent years the World Health Organization has endorsed the approach to address outbreaks of yellow fever, polio and other diseases.
“This is not an uncommon situation” said Dr. William Moss of Johns Hopkins’ Vaccine Access Center. “It comes down to the public health decision-making: In the midst of an outbreak where you have insufficient supply, do you make this tradeoff?”
When the first COVID-19 vaccines became available in late 2020, the U.K. government prioritized giving a first dose to as many people as possible before providing second vaccinations.
Both the U.K. and Canada have adopted a single-dose vaccine strategy prioritizing people who face the highest risk from monkeypox. And health departments in several large U.S. cities adopted a similar strategy amid limited supplies, including New York, San Francisco and Washington.
U.S. officials have shipped more than 617,000 full vaccine doses to state and local health departments and plan to distribute another 380,000 in coming weeks. So far it’s been recommended for people who have already been exposed to monkeypox or are likely to get it due to recent sexual contacts in areas where the virus is spreading.
The Biden administration has come under fire for not quickly marshaling millions more doses from the nation’s strategic national stockpile. Officials have ordered 5 million shots since July, but most aren't expected to be delivered until 2023.
The U.S. government owns bulk vaccine ingredients equivalent to 16.1 million doses under contracts with Danish manufacturer Bavarian Nordic. But the material needs to be sealed in vials, a process that’s expected to take months as the small company fields orders from other nations.
HHS responded to criticism last week about the pace and timing of the government’s vaccine decisions.
“We were thoughtful about how and when to use bulk vaccine because once you remove it from bulk, you lose years of shelf life,” a spokesperson said in an emailed statement.
The FDA approved the Jynneos vaccine in 2019 to prevent smallpox and monkeypox based, in part, on studies in monkeys. Animals that received the two-dose vaccination were more than twice as likely to survive than those who didn't after being infected with monkeypox, according to the FDA labeling.
Additional human studies showed people who received Jynneos had an immune response similar to those who received an older smallpox vaccine. But Jynneos hasn't been tested in humans with either monkeypox or its relative smallpox, which was eradicated decades ago.
That's typical of many of the vaccines and drugs in the national stockpile that treat rare or deadly pathogens like anthrax or the plague.
The U.S. government has spent more than $1 billion developing and stockpiling the freeze-dried vaccine, which replaced an earlier liquid version that had a shorter shelf life. Bavarian Nordic has a 10-year contract with the U.S. to supply the new vaccine.
___
The Associated Press Health and Science Department receives support from the Howard Hughes Medical Institute’s Department of Science Education. The AP is solely responsible for all content.